Acute low back pain can be debilitating. Nearly everybody, at some point in their life, will have acute back pain. It can come about for a variety of reasons. Sometimes a person will know why they have back pain; it snowed a foot and most of a Sunday afternoon might have been spent shoveling. It’s a classic case of doing something we are not accustomed to doing and being sore, maybe even a “good” sore for a few days afterward.

There are other times when it is unexplained and alarming. Over the years of practicing I’ve heard about many situations like the following.
- I turned to load the dishwasher and then I couldn’t stand up straight
- I was helping a friend move some furniture
- I moved the wrong way at the gym
- I took a new class at the gym with a friend. Now my back hurts.
- I slept wrong
- It just began hurting
- I was carrying my child
- I was washing the front door before a day of clients and am in excruciating pain now (This was me a few years ago!)
I want to walk you through scenarios involving acute low back pain. We’re talking about situations like the above, not chronic low back pain. However, chronic low back pain can go awry to where it becomes suddenly debilitating. This can be due to muscular imbalances that accumulate over time and finally there is a tipping point that is alarming.
Is it an emergency?
First off, evaluate how bad it is. Ask yourself if this is a medical emergency? If you experience the following symptoms you should seek immediate medical attention. The following come from Harvard Medical School
- back pain that occurs at the same time as a fever
- leg weakness that comes on abruptly or gets progressively worse
- numbness in the groin
- loss of bowel or bladder control
- pain that worsens instead of getting better
- inability to find a comfortable position for sitting or sleeping during times when you feel back pain
What to do if it’s not an emergency
In 2017 the American College of Physicians issued new guidelines around what to do regarding acute and sub-acute low back pain. Low back pain is one of the most common reasons for all physician visits in the U.S. Most Americans have experienced low back pain.¹ It is a fact that most people’s back pain will get better over time regardless of treatment. I took a continuing education course years ago from the late Robert King. He stated that we could hang a sign on our office stating “80% of all back pain cured here!” because a majority of back pain will get better even if you do nothing. And while that statement is not far off the mark, there are things we can do to get through an acute episode.
First off, movement will often make things better. Just getting out the door and walking around the block can be extremely helpful. Quite often, remaining stationery, immobile or sedentary will not be very helpful. Muscles that are in spasm often remain in spasm if we are in a seated position. Unless movement causes debilitating pain (see above) try and move as much as possible.
The evidence showed that acetaminophen was not effective at improving pain outcomes versus placebo. Low-quality evidence showed that systemic steroids were not effective in treating acute or sub-acute low back pain.¹
The primary recommendation from American College of Physicians is the following.
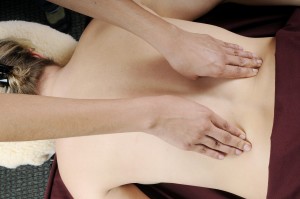
Recommendation 1:Given that most patients with acute or subacute low back pain improve over time regardless of treatment, clinicians and patients should select nonpharmacologic treatment with superficial heat (moderate-quality evidence), massage, acupuncture, or spinal manipulation (low-quality evidence). If pharmacologic treatment is desired, clinicians and patients should select nonsteroidal anti-inflammatory drugs or skeletal muscle relaxants (moderate-quality evidence). (Grade: strong recommendation)²
Personally, I am not a fan of using ice for low back pain. Using superficial moist heat as described above will feel better and allow a person to relax. Relaxing and moving the central nervous system away from “fight or flight” to “rest and relax” will facilitate healthy change in the body. Ice will cause a person to tense up, the opposite, in my opinion, of what I would want to achieve as a therapist. A note of caution however, be extremely careful not to burn yourself if using the microwave to warm a heat pack.
What if it is chronic?
Recommendation 2: For patients with chronic low back pain, clinicians and patients should initially select nonpharmacologic treatment with exercise, multidisciplinary rehabilitation, acupuncture, mindfulness-based stress reduction (moderate-quality evidence), tai chi, yoga, motor control exercise, progressive relaxation, electromyography biofeedback, low-level laser therapy, operant therapy, cognitive behavioral therapy, or spinal manipulation (low-quality evidence). (Grade: strong recommendation)²
I have experience with some of the suggestions in Recommendation 2 but not all of them. You’ll see that many include movement and relaxation techniques. Again, calming the body down is a primary goal. Breathing exercises will particularly help with this. I caution my clients, especially active or athletic clients to take it easy on stretching, especially aggressive static stretching. It is easy to overstretch a muscle and create new damage or increased damage to muscle fibers. Be patient and give the body time to settle down.
Where should you go first if you have acute low back pain?
If you are concerned that it is serious you should see your primary care doctor. Ask them if they think massage therapy or other suggested therapies would be helpful. Quite often, my clients will come to see me first. I will make an assessment and use some orthopedic tests to rule out a nerve root issue. I’ll look at muscular imbalance and if a muscle is unusually tight that may be contributing to the imbalance. My goal will be to get the client moving without compromise and hopefully without pain or with much reduced pain. They may leave still feeling some discomfort but things tend to get better quickly with movement and awareness around movement. I may offer a simple stretch or self-care technique to use at home.
The problem may not be resolved just because you are pain free. Remember, pain is a symptom. It is often the last symptom to show up and the first one to go away. Even though pain subsides it may be necessary to see a Physical Therapist for a thorough postural assessment to determine if strengthening exercises are needed to achieve an orthopedic balance in the body.
I’m never reluctant to refer out or ask for a second opinion. We have many brilliant, qualified health care professionals and I’ll use my network of referrals without hesitation. Don’t let back pain get you down. Slow down, listen to your body, keep moving and always feel free to call or email me if you have questions. I’ll do my best to help you figure out good steps toward feeling better.
Citations
.
